Date: 26 November 2013
Further details
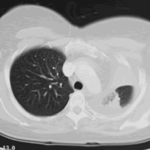
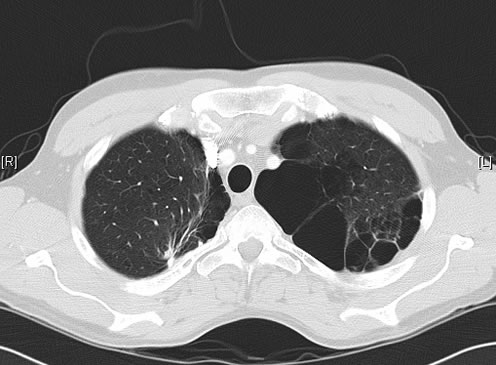
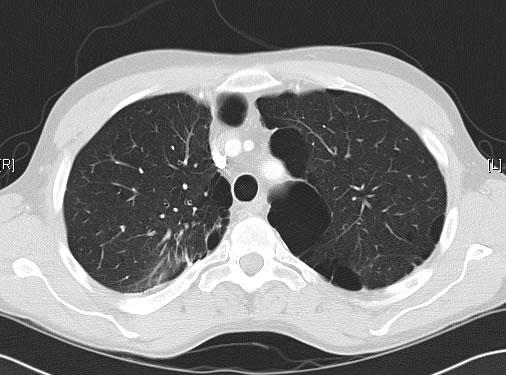
June 2009 – CT scan of the chest (two images D & E). These scans show residual large bullae, particularly notable in the apex of the left lung on both cuts. Small residual bullae remain in the right apex following a bullectomy which greatly reduced the size and number of these lesions.
Pt RK Lung bullae caused by cannabis smoking complicated by pneumothorax and chronic cavitary pulmonary aspergillosis.
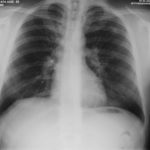
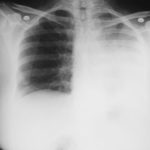
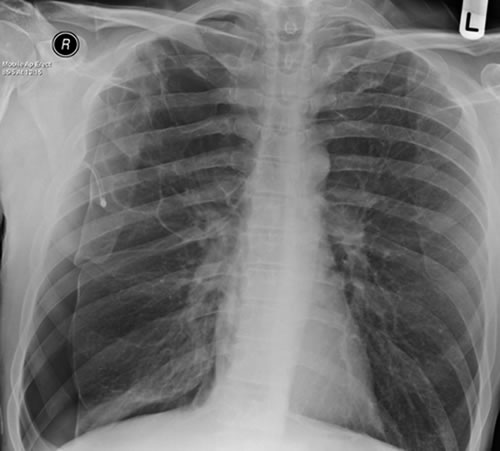
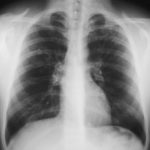
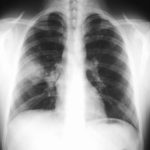
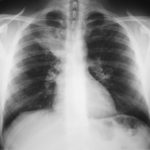
February 2009 – Chest x-ray showing bilateral apical bullae most marked on the right in association with a right pneumothorax. A chest drain is in-situ.
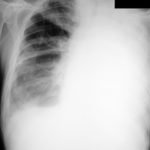
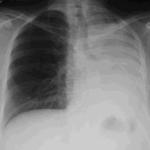
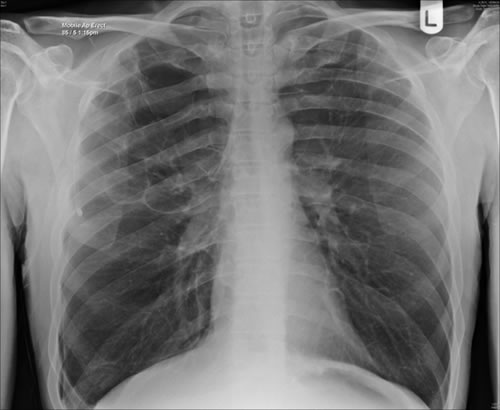
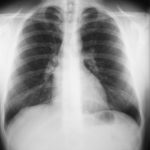
Late February 2009 – persistent apical bullae right upper zone with resolving pneumothorax. Chest drain still in-situ. Increasing right upper lobe shadowing possibly representing infection or haemorrhage.
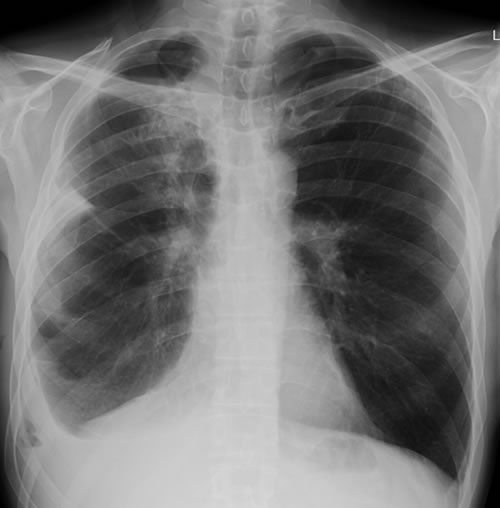
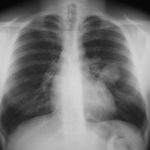
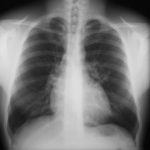
April 2009 – Post-operative chest x-ray showing post apical bullectomy on the right, resolved pneumothorax but the interval development of fluid in the right costo-phrenic angle with air fluid levels consistent with recent surgery. Great reduction in apical bullae in the right apex but increasing consolidation proximally in the right upper zone and some fluid in the horizontal fissure. These findings are following an apical bullectomy and pleurodesis of his prior significant pneumothorax.
June 2009 – CT scan of the chest (two images – see above). These scans show residual large bullae, particularly notable in the apex of the left lung on both cuts. Small residual bullae remain in the right apex following a bullectomy which greatly reduced the size and number of these lesions.
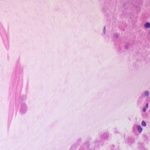
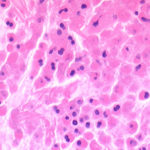
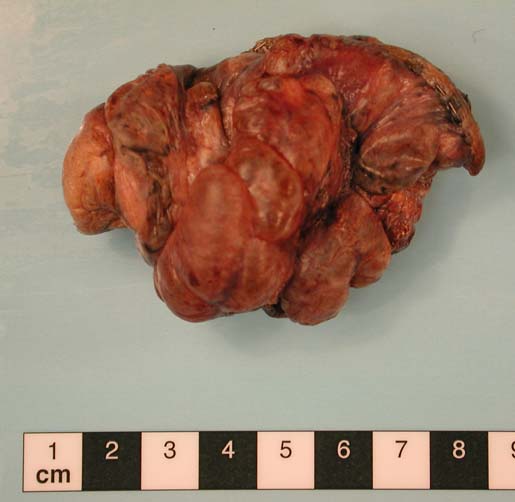
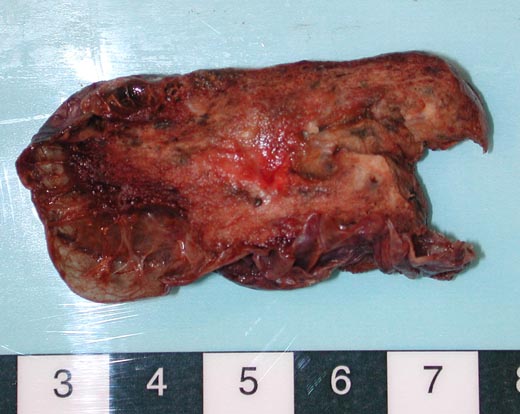
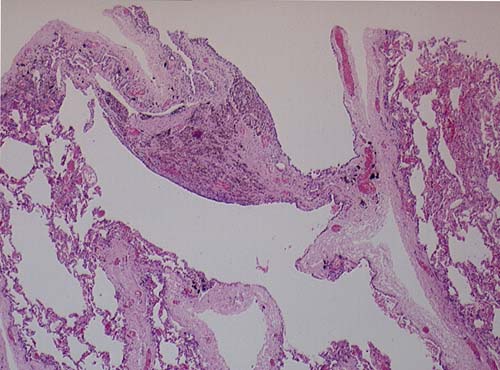
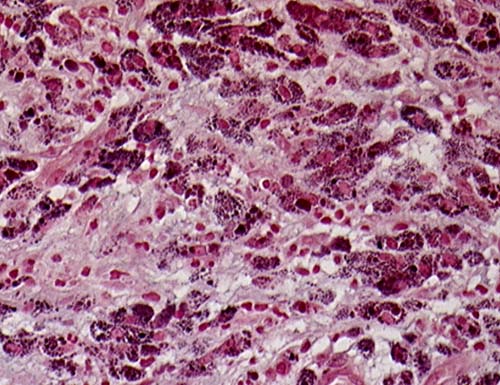
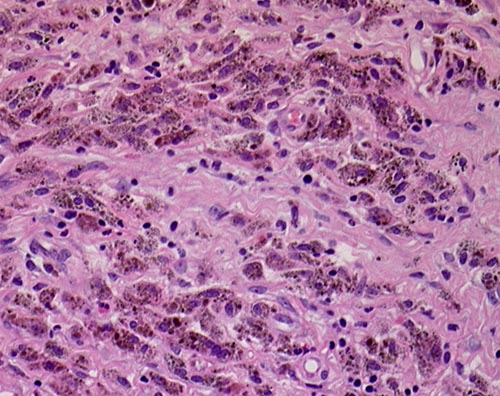
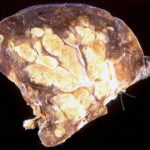
This patient underwent a bullectomy to remove part of the lung after developing lung bullae associated with cannabis smoking. The transverse section (G) of the specimen clearly shows the bullae along the left side and lower edge of the section. I and J demonstrate the dark pigment seen in accumulated macrophages. Tobacco smoking alone also causes a dark pigment, but evidence suggests that in marijuana smokers this pigment accumulates much faster and even with reduced exposure. The manner in which marijuana is smoked ie. without a filter and extended holding of the breath may contribute to this observation.
Copyright: n/a
Notes: n/a
Images library
-
Title
Legend
-
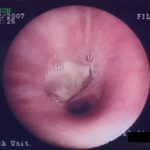
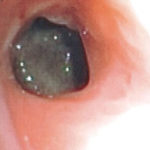
A. Necrotic mass prolapsing in and out of the distal right intermediate bronchus obscuring both the basal stem and basal division
-
History : A 20 yr old female with cystic fibrosis complicated by CF-related Diabetes mellitus (diagnosed at age 12 years) & ABPA (diagnosed at
15 years ). She was fairly stable until last 9 months, when she started to experience frequent pulmonary exacerbations, which have prompted intensive therapies.
Her serum IgE at the time of diagnosis was 5060 IU/L, skin prick test for aspergillus was positive, and serum was positive for precipitating antibodies to Aspergillus. She was treated with oral prednisone (1 mg/kg/day) for first two weeks followed by prednisone at 0.5 mg/kg every other day for at least 6 months with some clinical and serologic improvement. Over the following 5 years, she presented with a pattern of repeated episodic exacerbations with wheezing and crackles, increases in IgE and need to increase prednisone dosage. In an attempt to control her frequent ABPA relapses, itraconazole was added at 200mg twice a day, with some clinical & serologic improvement.
2-3 weeks prior to the scans and X rays, she developed severe protracted coughing spells associated with minor hemoptysis, low grade intermittent fever, and weight loss. Her FEV1 declined in a 3 months period from 56% to 33%.
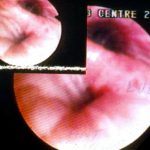
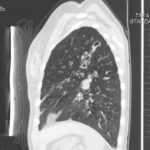
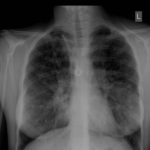
A chest-x ray (Fig 3) did not reveal any new changes when compared to the one obtained almost a year before. A CT scan of the chest Figs 1 and 2- lateral view), however shows an ovoid soft tissue density within an ectatic bronchi in the anterior basal segment of the LLL, felt to be an aspergilloma.She was started on oral voriconazole (3 months after the above scans and X-rays) which is better absorbed in CF patients than itraconazole, at 200mg twice a day. Her prednisone was gradually reduced to 5 mgs/day and her FEV1 increased to 46% of predicted (03/31/10), her IgE level was 1167 kU/L (previously in January 2009, her IgE level was 3053 kU/L)and her weight has plateaued.
Since she was not fit enough for surgery at that time, removing the aspergilloma by flexible bronchoscopy was unsuccessful. The aspergilloma can be seen at bronchoscopy in Fig 4. ,
,  ,
,  ,
, 
-
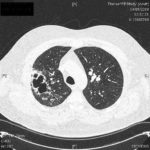
Widespread mucoid impaction also seen, particularly in left side, suggestive of allergic bronchopulmonary aspergillosis.
-
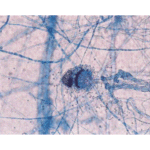
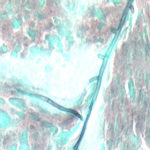
Microscopy of fungal hyphae isolated from fungal culture (lactophenol blue)
-
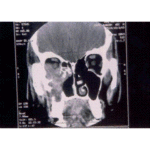
A CT scan performed at this time showed an enhancing lesion with ill defined margins involving the pterigopalatine fossa, the maxillary antrum , orbital apex and middle cranial fossa. There was also destruction of boney architecture locally.
-
The patient underwent a pneumonectomy because of the severity of her disease process, and uncertainty about the diagnosis, prior to serology results being obtained.
Serology showed an IgE of 2600, with a strongly positive Aspergillus RAST test and weakly positive Aspergillus precipitins. Material removed at bronchoscopy showed eosinophilia. These features confirm a diagnosis of allergic bronchopulmonary aspergillosis (ABPA).
 ,
,  ,
,  ,
,  ,
,  ,
,  ,
,  ,
,  ,
,  ,
, 

 ,
,  ,
,  ,
,  ,
,  ,
,  ,
,