Date: 26 November 2013
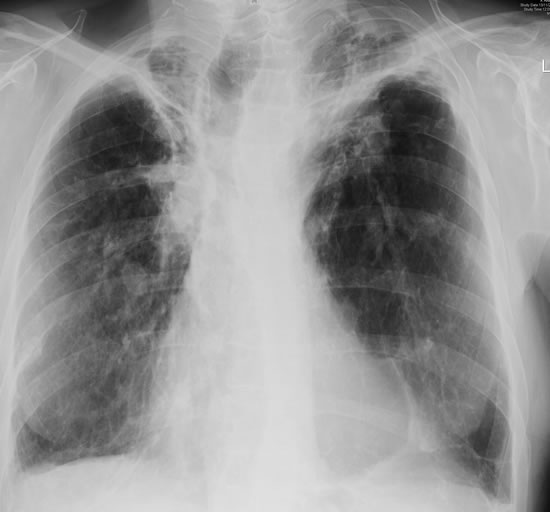
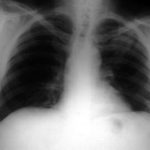
Born 75 years ago, Pt HK had 3 episodes of tuberculosis as a child and teenager, being treated with PAS and streptomycin. He suffered a ‘bad chest’ all his life and retired aged 54. Presenting with worsening and more frequent chest infections, he was referred with ‘bronchiectasis and Aspergillus sensitisation’. A diagnosis of chronic pulmonary aspergillosis was made in June 2009 on the basis of his chest radiograph and strongly positive Aspergillus precipitins (IgG antibodies) (titre 1/16). He also had Pseudomonas aeruginosa colonisation. His oxygen saturation was 87% and his pO2 6.8, pCO2 6.2 KPa.
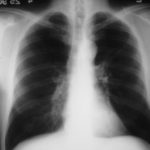
His chest radiograph (see above, November 2009) was reported as showing; “ The lung fields are over-inflated. Bilateral apical fibrotic change secondary to old TB. No cavity seen.” At clinic, bilateral apical cavities were seen, with some associated pleural thickening at the left apex, without any evidence of a fungal ball.
He started posaconazole 400mg twice daily with therapeutic levels at subsequent visits. Sputum cultures never grew Aspergillus. Over the following 9 months he had no chest infections requiring antibiotics, his breathlessness worsened gradually and he remained easily fatigued. His Aspergillus antibody titres fell. Overall he felt better, but was concerned about declining respiratory status.
Copyright:
Fungal Research Trust
Notes: n/a
Images library
-
Title
Legend
-
25/04/90 After itraconazole treatment. Major improvement, defined as a complete response, after 10 weeks therapy with itraconazole.
-
Image A. Chest x-ray shows a single nodule in the left mid lung field.
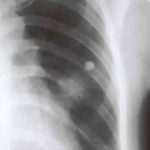
Image B. This emphasises how chest x-rays in this context underestimate the extent of disease. The most anterior nodule has ground glass surrrounding the nodule, a halo sign. This diagnostic feature is missed on plain chest X-rays.
 ,
, 
-
Chest X ray after 4 days, prior to treatment, showing massive increase in volume of lesion (Fig 2)
-
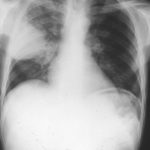
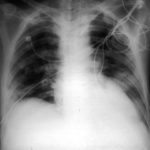
Image A. This patient, aged 25 years developed a non productive cough and dyspnoea in the context of late-stage AIDS, CMV disease with ganciclovir-induced neutropenia and receiving corticosteroids. His chest radiograph shows fine bilateral reticular lower-lobe shadowing. He then developed gastro-intestinal bleeding with a gastric ulcer which showed hyphae on biopsy. He then developed blindness of one eye and the globe of his eye perforated. Hyphae were seen and Aspergillus cultured from the vitreous aspirate.
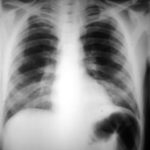
Image B. This radiograph, taken 25 days after the first and 3 days before death, shows of fine bilateral lower-lobe reticular shadows progressing to nodules in all lung zones.
This patient was reported as patient 3 in Denning DW, Follansbee S, Scolaro M, Norris S, Edelstein D, Stevens DA. Pulmonary aspergillosis in the acquired immunodeficiency syndrome. N Engl J Med 1991; 324: 654-662.
 ,
, 
-
Further details
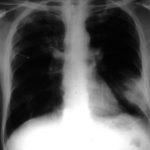
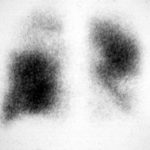
Image A. Bronchoscopy revealed Aspergillus on culture.
Image B. The ability of Aspergillus to cause pulmonary infarction, probably through direct angioinvasion in this case, is characteristic.
 ,
, 
-
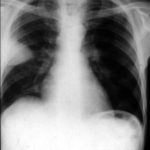
(Fig 1) Chest radiograph with ‘classical’ appearance of a pulmonary infarction – a wedge-shaped lesion peripherally set against the pleura.
-
Large soft left upper-lobe shadow of focal invasive pulmonary aspergillosis in leukaemia, that was missed on earlier radiographs but apparent retrospectively. Variable density of the lesion suggests cavitation, which would be clearly visible on a CT scan of the thorax.
-
Severe unilateral invasive aspergillosis of the left lung, with complete consolidation of the left lower-lobe and reticular shadowing extending up into the left upper lobe. The right lung appears normal.