Date: 26 November 2013
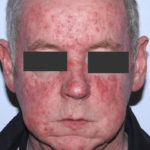
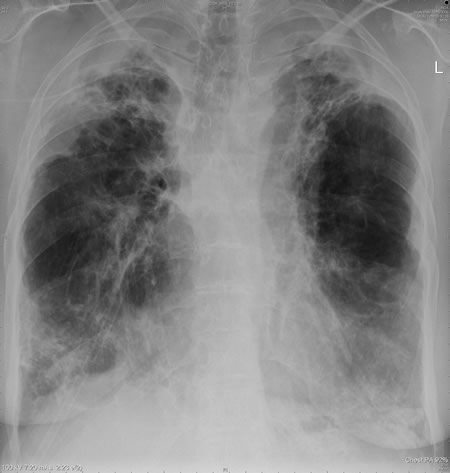
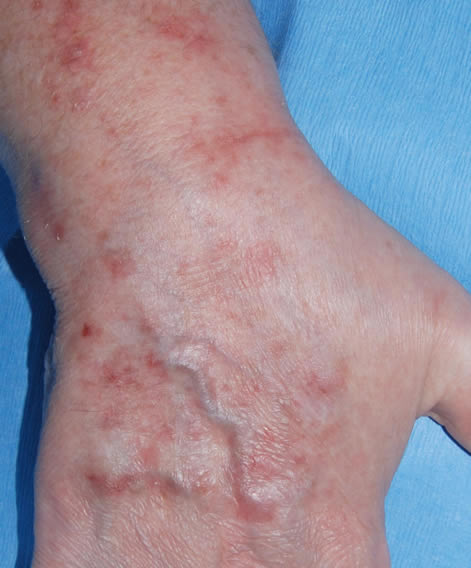
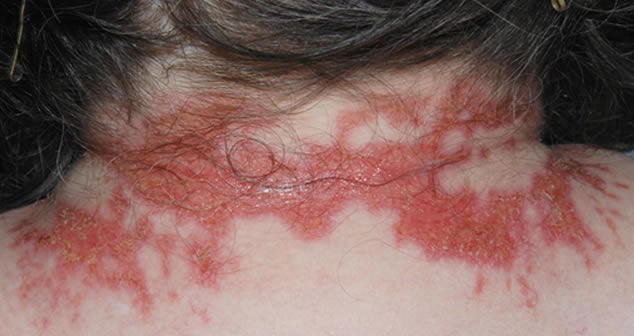
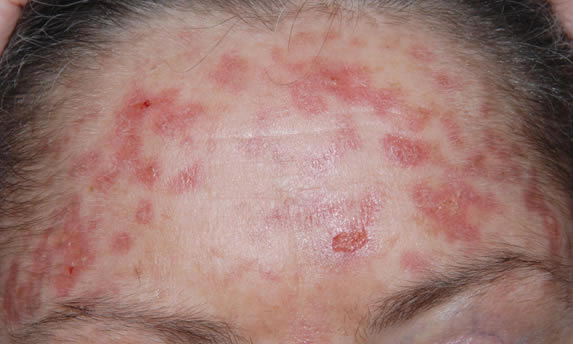
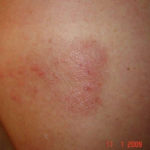
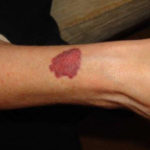
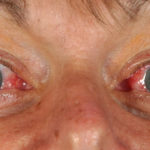
This patient with ABPA and chronic cavitary pulmonary aspergillosis has been stabilized on voriconazole treatment for >5 years. She had a degree of photosensitivity most of that time, noticed early in the course of voriconazole treatment. She is oxygen and wheelchair dependent and doesn’t go outside very much, so most of her light exposure has been indoor light. She developed rough scaly patches over her face, neck and lower arms. Dermatological review indicated multiple solar keratoses”. Skin biopsy from the right forearm confirmed this clinical diagnosis – “skin showing hyperkeratosis with a little parakeratosis and acanthosis. The keratinocytes have a glassy appearance but show nuclear atypia with dyskeratotic cells, and occasional suprabasal mitoses. The intraepidermal sweat ducts are spared. Appearances suggest an actinic keratosis with moderate to severe dysplasia.” These features are characteristic of a low grade premalignant change.
She was treated with local 5-fluorouracil cream (Efudix) (3 cycles) to the affected lesions. These photos were taken at the apogee of inflammation. The inflammation resolved after discontinuing the cream. This reaction is expected with application of this mild chemotherapy agent. Alternative or supplementary treatments include cryotherapy, curettage and cautery, if necessary. Following treatment her skin was much softer and considerably improved. Voriconazole has been stopped, and posaconazole substituted.
Copyright:
DW Denning and JE Ferguson, University Hospital of South Manchester. 22/07/08
Notes: n/a
Images library
-
Title
Legend
-
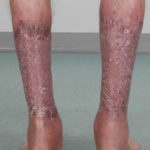
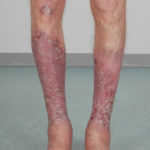
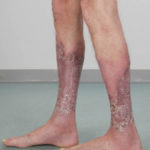
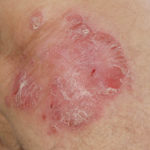
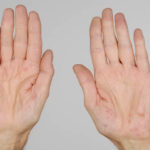
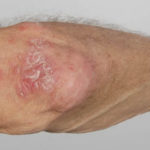
After 3 weeks of posaconazole given for chronic pulmonary aspergillosis, patient NC had a remarkable exacerbation of psoriasis. He had had psoriasis for years, with little trouble and almost no treatment. After taking posaconazole 400mg twice daily, he developed psoriatic plaques on his hands for the first time ever. The plaques on his lower legs became confluent. This occurred in association with worsening chest symptoms, notably increased coughing, more breathlessness and increasing oxygen requirement.
Posaconazole was stopped after 3 weeks, and 2 weeks later he was still very symptomatic with his chest. This responded to a 2 week course of corticosteroids, and his psoriasis also improved.
 ,
,  ,
,  ,
,  ,
,  ,
, 
-
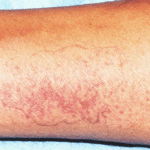
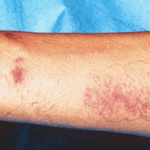
Patient PC: An example of localised caspofungin rash and phlebitis related to caspofungin infusion.
 ,
, 
-
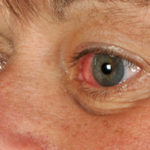
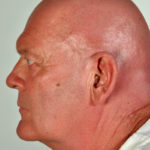
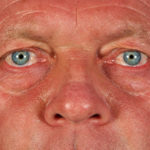
This 55 year old man with asthma, ABPA, severe bronchiectasis and lung fibrosis was treated with voriconazole, starting in June 2010. He had developed increasing dyspnoea on itraconazole for over 7 years, and his total IgE remained at 1100 KIU/L. He had marked photopsia (visual hallucinations) and facial erythema in the first 3 weeks of therapy. His trough voriconazole concentration was 1.17 mg/L. Over 3 months, he had minor improvement in his breathlessness but continued facial erythema, despite factor 50 sunblock. After 5 months of therapy his facial rash has altered to show acneiform lesions with localised crusting and background severe erythema. His face effectively crusted over, and he stopped therapy.
Over the next 3 weeks his facial appearance slowly improved .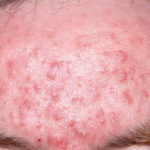 ,
,  ,
,