Date: 26 November 2013
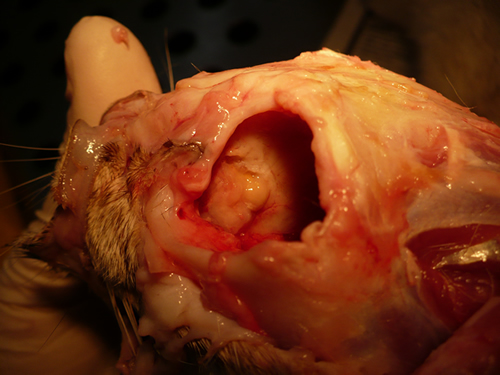
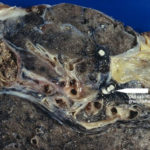
Nasal, sinus and orbital aspergillosis in a cat. The left nasal cavity and sinus were full of pus and debris and there was severe bone erosion from the nasal cavity into the rostromedial orbitthrough which pus was protruding
Copyright:
(Kindly provided by Martin L. Whitehead, BSc, PhD, BVSc, CertSAM, MRCVS & Peter W. Kettlewell, BVSc, MSc, MRCVS. Chipping Norton Veterinary Hospital, Albion Street, Chipping Norton, Oxon, OX7 5BN.)
Notes:
History : Nasal aspergillosis is relatively common in dogs but rare in cats. Our veterinary hospital in Oxfordshire was recently presented with a 13-year old female Burmilla cat with a history of left-side unilateral nasal discharge, a watery left eye with slight blepharospasm, occasional ‘twitching movements’ of the head, weight loss, inappetance and depression. Clinical examination was unremarkable except for left-side mucopurulent nasal discharge, left-side mild serous ocular discharge, and a soft subcutaneous swelling over the left frontal sinus. Haematology, blood biochemistry and urinalysis revealed diabetes mellitus but was otherwise unremarkable. Radiography under general anaesthesia revealed a diffuse soft tissue density within the left nasal cavity and left frontal sinus. Rhinoscopy revealed mucopurulent discharge on the left side but was otherwise unremarkable. Aspiration of the swelling over the left frontal sinus produced pus and this abscess was lanced and flushed. The frontal sinus was trephined and the sinus and nasal cavity flushed with saline. Tests for feline immunodeficiency virus and feline leukaemia virus and serology for Aspergillus were not carried out. The cat was started on insulin, ibafloxacin (Ibaflin, Intervet) and meloxicam (Metacam, Boehringer). Cytology of the material flushed from the frontal sinus and nasal cavity revealed fungal hyphae consistent with Aspergillus species and culture of this material yielded growth of a fungus which was morphologically similar to A. candidus (Awaiting molecular typing results). The cat was then started on oral itraconazole (Itrafungol, Janssen) 10 mg/kg p.o. SID. The abscess over the rostral frontal sinus did not heal and a second abscess appeared over the nasal bone just dorsal to the nose. Infusion of the frontal sinus and nasal cavity with topical antifungal medication was discussed with the owners, but as the cat was deteriorating they requested euthanasia. On post-mortem examination the right nasal cavity, frontal sinus and orbit were unaffected. The left nasal cavity and sinus were full of pus and debris and there was severe bone erosion from the nasal cavity into the rostromedial orbit through which pus was protruding. There was also severe bone erosion rostrally through the nasal bone and less severe bone erosion dorsally over the rostral part of the frontal sinus, these sites of bone erosion being at the location of the two subcutaneous abscesses.Feline nasal aspergillosis is extremely rare in the UK and to our knowledge this is the first reported case of orbital aspergillosis in the UK although nasal aspergillosis has been reported in other countries.
Images library
-
Title
Legend
-
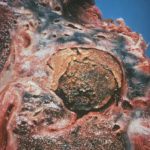
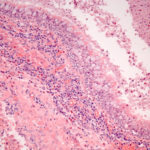
Macroscopic view medial aspect of left upper lobe of lung showing segmental collapse and congestion of lower segments, with mucus extruding from incised bronchi.
 ,
,  ,
,  ,
,  ,
, 
-
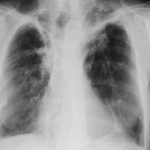
Born 75 years ago, Pt HK had 3 episodes of tuberculosis as a child and teenager, being treated with PAS and streptomycin. He suffered a ‘bad chest’ all his life and retired aged 54. Presenting with worsening and more frequent chest infections, he was referred with ‘bronchiectasis and Aspergillus sensitisation’. A diagnosis of chronic pulmonary aspergillosis was made in June 2009 on the basis of his chest radiograph and strongly positive Aspergillus precipitins (IgG antibodies) (titre 1/16). He also had Pseudomonas aeruginosa colonisation. His oxygen saturation was 87% and his pO2 6.8, pCO2 6.2 KPa.
His chest radiograph (see above, November 2009) was reported as showing; “ The lung fields are over-inflated. Bilateral apical fibrotic change secondary to old TB. No cavity seen.” At clinic, bilateral apical cavities were seen, with some associated pleural thickening at the left apex, without any evidence of a fungal ball.
He started posaconazole 400mg twice daily with therapeutic levels at subsequent visits. Sputum cultures never grew Aspergillus. Over the following 9 months he had no chest infections requiring antibiotics, his breathlessness worsened gradually and he remained easily fatigued. His Aspergillus antibody titres fell. Overall he felt better, but was concerned about declining respiratory status.